Breast Cancer
Introduction
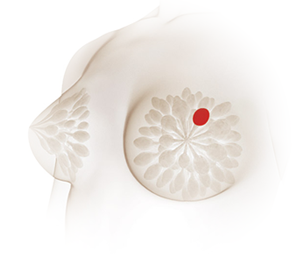
Breast cancer is the most common cancer among women in Singapore, accounting for around 30% of all female cancer diagnoses. 1 in 12 women will get breast cancer in their lifetime*.
Breast cancer usually originates from the cells lining the milk ducts and glands. When breast cancer is detected at this non-invasive or in-situ stage, treatment is easier and patients have a higher chance of recovery.
However, when cancer cells invade the surrounding tissue, known as the stroma, it can gain entry into the circulatory and lymphatic system, and hence, to other organs in the body, through the blood and lymphatic vessels found in the stroma. When these cancer cells reach a new site, they may form a metastatic tumour. The organs most commonly affected by this are the lungs, bones, and liver.
*Singapore Cancer Registry Annual Report 2023
Risk Factors
Age and Sex
The risk of breast cancer increases with age. Most women who are diagnosed to have breast cancer are older than 40 years old. However, younger women may also be affected.
Although breast cancer is much less common in men than in women, it can still occur. In men, it is often diagnosed at a more advanced stage due to smaller breast tissue, which makes early detection harder. Limited awareness and delayed recognition of symptoms also contribute to later diagnoses.
Family History
Certain genes have been identified and may be associated with the occurring of breast cancer, two of which are BRCA1 and BRCA2. A woman’s lifetime risk of developing breast cancer is greatly increased if she inherits an abnormal form of BRCA1 or BRCA2.
Woman with a first degree relative (i.e. mother, sister, or daughter) who has breast cancer is twice as likely to get breast cancer themselves, as compared to women without a family history of breast cancer. It is recommended woman with such a family history is to start breast cancer screening 10 years before the age of your relative’s diagnosis.
The likelihood of a woman in Singapore developing breast cancer in her lifetime is about 5%. However, those with a family history of breast cancer will have twice the risk compared with women without a family history.
Reproductive History
Certain aspects of a woman's reproductive history can increase her risk of breast cancer. These include:
• Not having children or having the first child after the age of 35
• Onset of menses before the age of 11
• Cessation of menses after the age of 55
These risk factors are associated with an early and prolonged exposure to oestrogen. To reduce risk, young girls below the age of 11 should be encouraged to exercise more as physical activity can delay the onset of menses and suppress the secretion of oestrogen. Breast-feeding, when carried out for more than a year, can also lower exposure to oestrogen and reduce a woman's risk of breast cancer.
Body Weight and Physical Activity
Weight gain, especially in post-menopausal women, is associated with an increased risk of breast cancer. This may be due to the combination of high calories and fat intake as well as a lack of exercise. Physical exercise reduces a woman's risk of breast cancer by lowering her body's level of oestrogen.
Women should engage in regular physical activities as well as moderate calories and fat intake to avoid weight gain.
Intake of Hormones
There are 2 groups of women whose intake of oestrogen and/or progesterone supplements may increase the risk of breast cancer.
- Post-menopausal women who are long term or current users of Hormone Replacement Therapy (HRT) have a 30% increased risk of breast cancer. This risk disappears after three to five years of stopping HRT. Women should engage in close discussion with their doctor(s) before making a decision.
- Young girls who consume oral contraceptive pills between the ages of 10-15
Diet
Excessive consumption of red meat, animal fat, and alcohol may increase a woman's risk of breast cancer. Women are encouraged to limit the intake of saturated animal fats and increase the intake of fruits and vegetables to reduce the risk of developing cancer. Besides, it is best not to drink alcohol.
Other nutrients that alter a woman's risk of breast cancer include:
- Soy products in bean curd and soya bean juice could reduce a woman’s risk of breast cancer
- Omega 3 oil from fish could reduce a woman’s risk from breast cancer
- Other nutrients that protect against breast cancer include Vitamin A, Selenium, and Vitamin C and E
Previous Abnormal Breast Biopsy
A few types of breast biopsy results may be indicative of an increased risk of breast cancer. Women whose biopsies indicate atypical ductal hyperplasia, atypical lobular hyperplasia, or lobular carcinoma in-situ should undergo regular breast screening.
Women with previous instances of breast cancer are also at an increased risk of developing cancer in the same or opposite breast and should seek regular screening.
Doctors can now provide a fairly good estimate of a woman's risk of breast cancer by tracing a detailed family, social, and medical history.
Women who are at high risk of breast cancer can take action by:
- starting breast screening at an earlier age
- altering lifestyle and diet to reduce risk
- taking Tamoxifen, an important anti-cancer drug, which can significantly reduce the risk of breast cancer
- undergoing preventive prophylactic mastectomies. Women at high-risk who underwent bilateral mastectomies had a 90% reduction of risk. However, given the extensive nature of the surgery involved, women are advised to carefully consider their options. Despite the above list of risk factors, the exact cause of breast cancer remains unknown. About 50 per cent of breast cancer patients have no identifiable risk factors.
Signs & Symptoms
Common signs and symptoms of breast cancer may include:
- Breast lumps
- Bloody nipple discharge
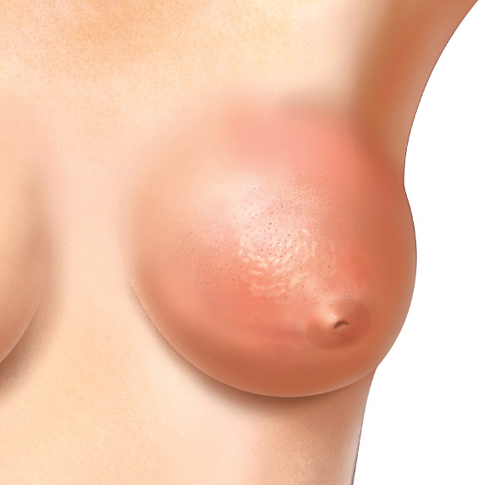
- Skin changes
- Itchy rash of the nipple
- Breast pain
8 out of 10 breast lumps are benign or non-cancerous. There are different classifications of breast lumps that can occur, depending on a woman's age.
Women in Their 20s
The most commonly occurring type of breast lump in this age group is a fibroadenoma. It is also known as a breast ‘mouse' as it can be moved within the breast. It is non-cancerous.
Women in Their 30s
The most common type of breast lump for women in this age group is fibroadenosis or fibrocystic disease. It is often a painful hard area in the outer area of the breast and is associated with the female sex hormone oestrogen. It is non-cancerous.
Women in Their 40s and Beyond
Two types of breast lumps are common in older women. One is a breast cyst which is a lump filled with fluid. Breast cysts can be diagnosed by an ultrasound scan and is treated by a needle puncture to extract the fluid. The other type of breast lumps that commonly occur in older women are due to breast cancer. Cancerous breast lumps are usually hard, irregularly shaped, and occupy a fixed position inside the breast. Changes in the skin over the cancerous lump may be observed, such as skin thickening, redness, soreness, and/or depression.
Early Detection & Screening
Early detection significantly increases the chances of surviving breast cancer. Early detection is facilitated by regular screening such as mammograms and monthly breast self-examinations.
For women aged 20 and above, it is recommended to perform a monthly breast self-examination to become familiar with the normal feel and appearance of their breasts. This practice helps in the early identification of any unusual changes or lumps that should prompt medical consultation.
For women aged 40 and above, you recommended to go for mammogram screening. The mammogram is currently the most reliable screening tool for breast cancer. It can detect the presence of cancerous lumps even before they can be felt with the hand.
Diagnosis
Diagnosis of breast cancer is based on:
- Clinical examination
- Mammography
- Ultrasound scan of the breast
To confirm the diagnosis, a breast biopsy is performed to remove a piece of tissue for examination under a microscope.
Common biopsy techniques include:
- Fine Needle Aspiration (FNA)
- Core Needle Biopsy
- Excision Biopsy
- Sentinel Lymph Node Biopsy (SLNB)
Treatment
Mastectomy
A mastectomy entails the removal of the whole breast, including the nipple.
Lumpectomy
A lumpectomy entails the removal of a tumour along with a margin of normal breast tissue. This leaves the rest of the breast untouched. After a lumpectomy, radiotherapy is given to the breast for 6 weeks. This treatment is safe and has a low recurrence rate. Breast cancer patients who are suitable for lumpectomy and radiotherapy have:
- Tumours situated away from the nipple
- Tumours less than 2-3 cm in diameter
- Breasts of a suitable size
Breast cancer patients are not suitable for a lumpectomy if they:
- Are under the age of 30 due to a high recurrence rate
- Are pregnant
- Have connective tissue disease
- Have 2 or more tumours within the same breast
Armpit Surgery
Armpit surgery is required to remove the axillary lymph nodes for diagnostic and therapeutic purposes. Knowing whether cancer has entered the axillary lymph nodes is important in determining the stage of breast cancer. Removal of the axillary lymph nodes also prevents the recurrence of cancer in this area. Some breast cancer patients may experience temporary shoulder stiffness and arm swelling after this procedure.
Sentinel Lymph Node Biopsy (SLN Biopsy)
1 or 2 lymph nodes act as a gateway to the axilla and will be the first to be affected should cancer enter this area of the body. By identifying and biopsying these sentinel lymph nodes, it can be determined whether the rest of the axillary lymph nodes are affected by cancer.
SLN biopsy is a viable treatment option for patients with:
- Small tumours
- Non-palpable nodes in the axilla
SLN biopsy is not recommended for:
- Patients with large tumours and palpable nodes, who should undergo an axillary dissection
- Patients with non-invasive tumours, for whom no axillary surgery is required
Post-Mastectomy Breast Reconstruction
Following a mastectomy, breast reconstruction can be carried out using a variety of techniques. The following considerations may be important to note:
- Timing of Reconstruction
- Cost and Complications
The breast can be reconstructed using an artificial implant (usually made of silicon) or a skin-muscle flap from the patient’s own body. An artificial implant is quicker and cheaper to undertake but some women may be averse to the presence of a foreign object in their body.
Extracting a skin-muscle flap from the patient is a natural method for breast reconstruction but is longer and costlier to undertake. This method may also lead to complications surrounding the area where the skin-muscle is taken. - Cancer Recurrence
An artificial implant or a reconstructed breast has not been found to interfere with the detection of cancer recurrence or to increase the risk of cancer recurrence.
Radiotherapy
Radiotherapy utilises radiation to treat breast cancer. Radiotherapy is recommended for the local treatment of breasts following a lumpectomy. It is given over 6 weeks during daily outpatient treatment sessions. Side effects are usually tolerable and mainly confined to the treatment area. Radiotherapy is also recommended for women after mastectomy whose risk of local recurrence is high and whose lymph nodes and tumours are more than 4cm wide.
Cytotoxic Chemotherapy
This involves the administration of toxic drugs which are harmful to both cancer cells and healthy cells. Given their toxicity, the drugs are administered at controlled dosages over a period of time to limit their toxicity while eliminating cancer cells.
There are 3 main regimes, each consisting of a combination of cytotoxic drugs. Depending on the condition and needs of the patient, the most suitable regime is selected and administered at 3 weekly intervals over 4 to 6 months.
The following list of short-term side effects resulting from chemotherapy may be severe but are usually tolerable and temporary.
- Low total white cell count (Less than 2000/mm3)
- Fever
- Infection
- Nausea
- Diarrhoea
- Hair loss
- Low platelet count (Less than 50,000/mm3)
- Blood clots in veins
- Cystitis
- Weight gain (More than 10%)
Although these are significant side effects associated with cytotoxic chemotherapy, the mortality rate resulting from chemotherapy is low. Nevertheless, in very sick patients, death may result from overwhelming infection or the formation of blood clots in veins.
3 major long-term side effects associated with chemotherapy have been identified:
- Premature menopause – A woman in her forties has a 50 per cent chance of experiencing premature menopause if she undergoes chemotherapy. The effects of menopause are more severe in younger women, varying from hot flushes, palpitations, and dry skin to more debilitating conditions such as osteoporosis and increased risk of cardiovascular disease.
- Cardiac toxicity – Adriamycin (or Doxorubicin) is a common drug component of chemotherapy that can cause heart failure. However, the probability of experiencing this side effect is low and can be decreased by:
1. Assessing cardiac function
2. Limiting the dose administered
3. Calibrating the method of drug administration - Risk of a second cancer – Rare instances of chemotherapy-induced leukaemia have been recorded.
Hormonal Manipulation
This entails altering or stopping the secretion of oestrogen in the patient's body as a means of treating breast cancer through the use of Tamoxifen. It is taken orally once a day and causes few side effects. It is effective for:
- Women at high risk of breast cancer and is taken as a preventive drug.
- Women whose breast cancer is oestrogen receptor positive (ER+) and is at low risk of recurrence. Tamoxifen is given as the sole systemic drug.
- Women whose breast cancer is ER+ and is at high risk of recurrence. Tamoxipfen is combined with chemotherapy or other measures of hormonal manipulation.
Ovarian Ablation
This refers to methods to stop the secretion of oestrogen in a woman's body in order to reduce the stimulation of cancer cells and hence reduce the chance of cancer recurrence. This method applies only to pre-menopausal women and leads to premature menopause. Ovarian ablation can be achieved by surgical or non-surgical methods:
- Surgical Oophorectomy – Surgery is undertaken to permanently remove the ovaries. This method is now seldom used.
- Radiation Castration – Radiotherapy is given to patients over a 2 week period to permanently disable the ovaries from secreting oestrogen. This is a quick and relatively painless method.
- Ovarian Suppression – The secretion of oestrogen is controlled by the pituitary gland. Drugs can be prescribed to temporarily suppress oestrogen secretion. Ovarian function usually recovers once the drug is stopped. This is a relatively expensive method.

